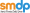Surgeons transplanted a pig’s kidney into a brain-dead man and for over a month it worked normally — a critical step toward an operation the New York team hopes to eventually try in living patients.
Scientists around the country are racing to learn how to use animal organs to save human lives, and bodies donated for research offer a remarkable rehearsal.
The latest experiment announced Wednesday by NYU Langone Health marks the longest a pig kidney has functioned in a person, albeit a deceased one -– and it’s not over. Researchers are set to track the kidney’s performance for a second month.
"Is this organ really going to work like a human organ? So far it’s looking like it is," Dr. Robert Montgomery, director of NYU Langone’s transplant institute, told The Associated Press.
"It looks even better than a human kidney," Montgomery said on July 14 as he replaced a deceased man’s own kidneys with a single kidney from a genetically modified pig — and watched it immediately start producing urine.
The possibility that pig kidneys might one day help ease a dire shortage of transplantable organs persuaded the family of Maurice "Mo" Miller from upstate New York to donate his body for the experiment. He died suddenly at 57 with a previously undiagnosed brain cancer, ruling out routine organ donation.
"I struggled with it," his sister, Mary Miller-Duffy, told the AP about her decision. But he liked helping others and "I think this is what my brother would want. So I offered my brother to them."
"He’s going to be in the medical books, and he will live on forever," she added.
Attempts at animal-to-human transplants, or xenotransplantation, have failed for decades as people’s immune systems attack foreign tissue. Now researchers are using pigs genetically modified so their organs better match human bodies.
Last year with special permission from regulators, University of Maryland surgeons transplanted a gene-edited pig heart into a dying man who was out of other options. He survived only two months before the organ failed for reasons that aren’t fully understood but that offer lessons for future attempts.
Next, rather than last-ditch efforts, the Food and Drug Administration is considering whether to allow some small but rigorous studies of pig heart or kidney transplants in volunteer patients.
The NYU experiment is one of a string of developments aimed at speeding the start of such clinical trials. Also Wednesday, the University of Alabama at Birmingham reported another important success — a pair of pig kidneys worked normally inside another donated body for seven days.
Kidneys don’t just make urine — they provide a wide range of jobs in the body. In the journal JAMA Surgery, UAB transplant surgeon Dr. Jayme Locke reported lab tests documenting the gene-modified pig organs’ performance. She said the weeklong experiment demonstrates they can "provide life-sustaining kidney function."
These kinds of experiments are critical to answer remaining questions "in a setting where we’re not putting someone’s life in jeopardy," said Montgomery, the NYU kidney transplant surgeon who also received his own heart transplant — and is acutely aware of the need for a new source of organs.
More than 100,000 patients are on the nation’s transplant list and thousands die each year waiting.
Maryland’s Dr. Muhammad Mohiuddin cautions that it’s not clear how closely a deceased body will mimic a live patient’s reactions to a pig organ. But he said the research educates the public about xenotransplantation so "people will not be shocked" when it’s time to try again in the living.
Previously, NYU and a team at the University of Alabama at Birmingham had tested pig kidney transplants in deceased recipients for just two or three days. An NYU team also had transplanted pig hearts into donated bodies for three days of intense testing.
But how do pig organs react to a more common human immune attack that takes about a month to form? Only longer testing might tell.
The surgery itself isn’t that different from thousands he’s performed "but somewhere in the back of your mind is the enormity of what you’re doing ... recognizing that this could have a huge impact on the future of transplantation," Montgomery said.
The operation took careful timing. Early that morning Drs. Adam Griesemer and Jeffrey Stern flew hundreds of miles to a facility where Virginia-based Revivicor Inc. houses genetically modified pigs — and retrieved kidneys lacking a gene that would trigger immediate destruction by the human immune system.
As they raced back to NYU, Montgomery was removing both kidneys from the donated body so there’d be no doubt if the soon-to-arrive pig version was working. One pig kidney was transplanted, the other stored for comparison when the experiment ends.
One other trick: Surgeons attached the pig’s thymus to the transplanted kidney in hopes that the gland, which helps train immune cells, would increase human tolerance of the organ. Otherwise, the team is relying on standard immune-suppressing drugs used by today’s transplant patients.
"You’re always nervous," Griesemer said. To see it so rapidly kickstart, "there was a lot of thrill and a lot of sense of relief."
How long should these experiments last? Alabama’s Locke said that’s not clear -– and among the ethical questions are how long a family is comfortable or whether it’s adding to their grief. Because maintaining a brain-dead person on a ventilator is difficult, it’s also dependent on how stable the donated body is.
In her own experiment, the donated body was stable enough that if the study wasn’t required to end after a week, "I think we could have gone much longer, which I think offers great hope," she said.
LAURAN NEERGAARD, AP Medical Writer
AP video journalist Shelby Lum contributed to this report. The Associated Press Health and Science Department receives support from the Howard Hughes Medical Institute’s Science and Educational Media Group.